Long-term Management of Skin Sensitivity
Skin sensitivity and persistent itching can significantly impact daily life, affecting sleep quality, work productivity, and overall well-being. Understanding the underlying causes of chronic skin irritation is essential for developing effective management strategies. From environmental triggers to underlying medical conditions, various factors contribute to long-term skin sensitivity. This comprehensive guide explores proven approaches to managing persistent skin issues, including natural remedies, medical treatments, and lifestyle modifications that can provide lasting relief.
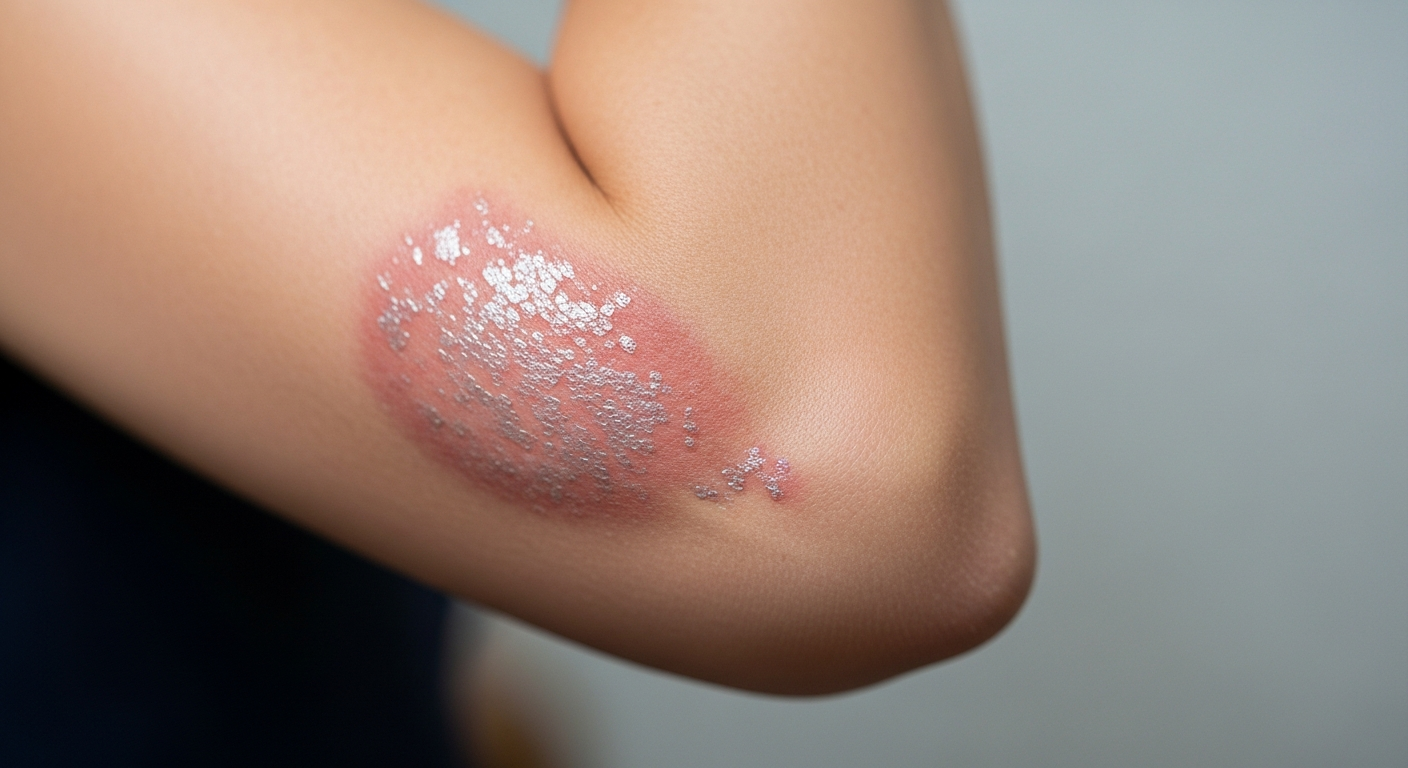
Managing chronic skin sensitivity requires a multifaceted approach that addresses both immediate symptoms and underlying causes. Unlike temporary irritation, persistent skin sensitivity often stems from complex interactions between genetic predisposition, environmental factors, and immune system responses.
Skin sensitivity manifests differently across individuals, ranging from mild occasional itching to severe, persistent discomfort that disrupts daily activities. Common symptoms include redness, dryness, burning sensations, and the overwhelming urge to scratch. Understanding these patterns helps identify triggers and develop personalized management strategies.
Ways to Get Rid of Itchy Skin Through Lifestyle Changes
Effective long-term management begins with identifying and eliminating triggers. Common culprits include harsh soaps, synthetic fabrics, extreme temperatures, and certain foods. Maintaining a symptom diary helps track patterns and identify specific triggers unique to each individual.
Moisturizing routines play a crucial role in managing skin sensitivity. Applying fragrance-free, hypoallergenic moisturizers immediately after bathing helps lock in moisture and strengthen the skin barrier. Choose products containing ceramides, hyaluronic acid, or glycerin for optimal hydration.
Environmental modifications can significantly reduce symptoms. Using humidifiers during dry seasons, choosing breathable cotton clothing, and maintaining comfortable room temperatures help minimize irritation. Additionally, stress management through regular exercise, meditation, or yoga can reduce symptom flare-ups.
Home Remedies for Itchy Skin That Provide Natural Relief
Several natural approaches offer gentle, effective relief for sensitive skin. Oatmeal baths have anti-inflammatory properties that soothe irritated skin. Adding finely ground oatmeal to lukewarm bathwater creates a protective film that reduces itching and inflammation.
Cold compresses provide immediate relief by numbing the affected area and reducing inflammation. Apply clean, damp cloths to irritated areas for 10-15 minutes several times daily. Avoid ice directly on skin, as extreme cold can worsen sensitivity.
Aloe vera gel offers natural moisturizing and anti-inflammatory benefits. Choose pure aloe vera without added fragrances or alcohol. Coconut oil also provides antimicrobial properties while moisturizing dry, sensitive skin. However, patch test any new topical treatment before widespread application.
Chamomile tea compresses can reduce inflammation and provide calming effects. Brew strong chamomile tea, allow it to cool, then apply with clean cloths to affected areas.
Medications for Itchy Skin and Professional Treatment Options
When natural remedies prove insufficient, various medications can provide relief. Topical corticosteroids, available in different strengths, reduce inflammation and itching. Over-the-counter options like hydrocortisone work well for mild symptoms, while prescription-strength formulations address more severe cases.
Antihistamines help manage itching by blocking histamine responses. Non-drowsy options like loratadine or cetirizine work well for daytime use, while sedating antihistamines like diphenhydramine can provide nighttime relief and improve sleep quality.
Topical calcineurin inhibitors, such as tacrolimus or pimecrolimus, offer alternatives to steroids for long-term management. These prescription medications effectively reduce inflammation without the side effects associated with prolonged steroid use.
For severe cases, dermatologists may prescribe systemic medications including oral corticosteroids, immunosuppressants, or newer biologic treatments targeting specific inflammatory pathways.
| Treatment Type | Examples | Typical Cost Range | Availability |
|---|---|---|---|
| Over-the-counter topicals | Hydrocortisone cream, Moisturizers | $5-$25 | Widely available |
| Prescription topicals | Stronger corticosteroids, Calcineurin inhibitors | $30-$200 | Prescription required |
| Oral antihistamines | Loratadine, Cetirizine | $10-$30 | Over-the-counter |
| Prescription oral medications | Prednisone, Immunosuppressants | $50-$500+ | Prescription required |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Prevention Strategies for Long-term Success
Preventing flare-ups requires consistent daily care routines. Gentle cleansing with lukewarm water and mild, fragrance-free cleansers helps maintain skin barrier function. Pat skin dry rather than rubbing, and apply moisturizer while skin is still slightly damp.
Dietary considerations may impact skin sensitivity. Some individuals benefit from eliminating common triggers like dairy, gluten, or processed foods. However, dietary changes should be made gradually and preferably under professional guidance.
Regular dermatological check-ups help monitor skin health and adjust treatment plans as needed. Professional evaluation ensures proper diagnosis and prevents complications from self-treatment.
When to Seek Professional Help
Consult healthcare providers when symptoms persist despite consistent self-care, worsen over time, or interfere with sleep and daily activities. Signs requiring immediate attention include signs of infection, widespread rash, or severe pain.
Dermatologists can perform patch testing to identify specific allergens, prescribe stronger medications, and rule out underlying conditions like eczema, psoriasis, or contact dermatitis.
Successful long-term management of skin sensitivity combines understanding personal triggers, consistent daily care, appropriate use of treatments, and professional guidance when needed. With patience and the right approach, most individuals can achieve significant improvement in their skin comfort and overall quality of life.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.




